MRSA, also known as Methicillin-Resistant Staphylococcus Aureus, is a notorious bacterium that has gained repute for its resistance to standard antibiotics such as penicillin and amoxicillin. This resistance has made MRSA infections difficult to treat and poses a significant health risk. In the quest for effective treatments, attention is focusing on a potential natural solution – mānuka oil.
An Overview of Mānuka Oil

Mānuka oil, scientifically known as Leptospermum scoparium and indigenous to New Zealand, has a rich history steeped in therapeutic, anti-inflammatory, antibacterial, antiviral, and antifungal properties. This essential oil can be employed topically in diluted form.
Mānuka oil is obtained through the gentle steam distillation of mānuka brush sustainably harvested from the East Cape region of New Zealand. This oil has garnered a reputation as an exemplary treatment for impetigo and numerous common skin staph infections. In fact, rigorous scientific investigations have unambiguously established the outstanding effectiveness of East Cape mānuka leaf oil in combating a wide range of staph bacteria. Consequently, it has become a formidable ally in the fight against these infections.
Mānuka Oil’s Secret Ingredient: Triketones
Among all the regions where harvesters cultivate mānuka, none surpasses the rural East Cape region of New Zealand in terms of the triketone content. Scientific validation of the exceptional triketone profile of oil from the East Cape identifies it as beneficial for skin health. These triketones within the oil exhibit potent antibacterial and antioxidant properties. Moreover, they play a crucial role in promoting anti-inflammatory effects, facilitating skin healing, and enhancing the turnover of skin cells. This unique combination of attributes underscores the therapeutic potential of East Cape mānuka oil in skincare.
Is Mānuka Oil Stronger Than Mānuka Honey?
Mānuka oil, while not as widely recognised as its honey counterpart, is increasingly gaining prominence as a powerful defence against the detrimental effects of MRSA. While many are familiar with the antibacterial properties of mānuka honey, a lesser-known fact is that mānuka oil is approximately 1,000 times more effective than mānuka honey in combating common skin bacteria, including staph infections.
Of noteworthy significance, mānuka oil exhibits exceptional cytophylactic (the ability of an oil to generate new cells, thus protecting the cells and preserving skin health) properties, facilitating cellular regeneration, and possesses cicatrizant attributes, making it an effective agent for antimicrobial purposes and tissue repair. Its potential as a formidable remedy in combating MRSA warrants further exploration and consideration.
Understanding MRSA
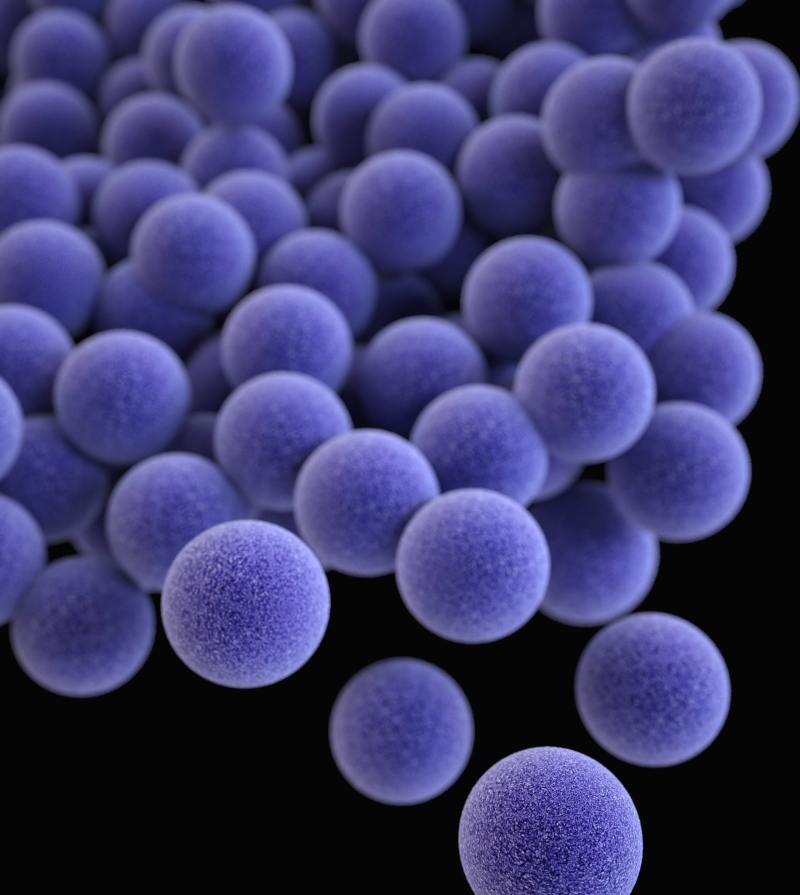
Methicillin-resistant Staphylococcus aureus (MRSA) infection results from a particular strain of staph bacteria that has developed resistance to many antibiotics typically employed to treat common staph infections.
What Is Staph?
Staphylococcus aureus (commonly known as Staph) bacteria are usually present on the skin and mucous membranes in a significant portion of the population, estimated to range from 20% to potentially exceeding 50% in some studies. Generally, Staph is regarded as benign in its interactions with humans. However, it is worth noting that the human immune system lacks a built-in defence mechanism against Staph, which can facilitate the bacteria’s dissemination throughout the body, posing a considerable and potentially severe health hazard.
Staph infections have the potential to spread more rapidly and present an increased risk in individuals with compromised immune systems.Factors including alcohol consumption, drug use, vitamin deficiencies, stress, fatigue, illness, and similar conditions can weaken the immune system. These factors make individuals more susceptible to the rapid proliferation and increased threat of Staph infections.
Staph Infections
Most skin infections are attributed to a group of microorganisms called Staphylococcus or staph bacteria. Bacterial skin infections can affect anyone, but certain individuals are more susceptible, including children, pregnant women, the elderly, individuals involved in contact sports, those residing in communal environments, individuals with a history of skin trauma, chronic ailments such as diabetes and heart disease, and those with compromised immune systems.
Normally, Staph bacteria coexist harmlessly on the skin and within the nasal passages of most healthy individuals. However, when the skin becomes compromised due to wounds, abrasions, or even minor cuts (such as paper cuts), these bacteria can proliferate rapidly, leading from mild to severe infections and, in some cases, life-threatening.
Common Staph infections with mild to moderate symptoms include impetigo, sties, abscesses, boils, folliculitis, cellulitis, carbuncles, and furuncles. Many of these ailments are contagious, causing extreme discomfort and severe pain. Early intervention is crucial in managing these infections.
In more severe cases, Staph infections can escalate to life-threatening levels if the bacteria infiltrate deeper into the body, gaining access to the bloodstream, joints, bones, lungs, or heart. Such serious and potentially fatal bacterial infections include:
- toxic shock syndrome
- endocarditis (inflammation of the heart valve)
- surgical wound infections
- septicaemia (blood poisoning)
- necrotizing fasciitis (a severe bacterial tissue disease)
- infections related to prosthetic devices such as heart valves, pacemakers, catheters, and joint replacements
What Is Impetigo?
Impetigo, known by various names such as skin sores, school sores, or pyoderma, is a highly contagious staph infection of the skin that afflicts approximately 162 million individuals worldwide each year. This condition is particularly prevalent among children under the age of five.
Notably, untreated impetigo is the only skin ailment capable of leading to life-threatening complications, including serious kidney and heart conditions such as rheumatic heart disease and chronic kidney disease. Hence, timely intervention is of paramount importance in managing this condition and preventing its potentially grave consequences.
Methicillin-Resistant Staphylococcus Aureus (MRSA)
Methicillin-Resistant Staphylococcus Aureus (MRSA) can pose a significant health risk, even to individuals in good health. MRSA exhibits a high degree of resistance to antibiotics and has the potential to be life-threatening. The emergence of MRSA is primarily attributed to the excessive prescription and overuse of antibiotics, making it a pressing concern, particularly within the healthcare sector.
The Centers for Disease Control and Prevention (CDC) reveals that MRSA carriers comprise less than 2 percent of the population at any given time. While this figure may seem relatively low, it becomes concerning when considering the number of individuals we encounter daily in various settings, including schools, hospitals, movie theatres, sporting events, restaurants, grocery stores, and workplaces. These are environments where people frequently touch surfaces such as door handles, light switches, countertops, and more. The reality is that we all come into contact with numerous germs, including MRSA, on a daily basis.
Research has indicated that MRSA can survive on inanimate objects, such as windows, door handles, light switches, and countertops, for several days. This underscores the importance of practising proper hygiene and infection control measures to minimize the risk of MRSA transmission.
How Is MRSA Transmitted?
The transmission of infections, including those caused by Staphylococcus bacteria, can occur through various means, primarily involving physical contact and exposure to contaminated surfaces:
- Physical contact with others: Infections can spread through activities such as handshakes, hugs, physical sports, and sexual contact when there is direct skin-to-skin contact with an infected individual.
- Contact with contaminated public items: Infections can be contracted by touching surfaces or items in public spaces, such as door handles, countertops, gas pumps, or packages at stores, that have been contaminated by infected individuals.
- Contact with household items: Infections can also be acquired within the home environment through contact with everyday items such as bath towels, light switches, washcloths, clothing, bed sheets, faucet handles, and similar objects that may carry bacteria if not properly sanitized.
- Congested environments: The risk of transmission is often higher in crowded or congested settings, including hospitals, locker rooms, schools, and other places where close contact and shared spaces can facilitate the spread of infections.
Who Are Most Susceptible to Contracting MRSA?
Most MRSA infections are observed in individuals who have spent time within healthcare settings, including hospitals, nursing homes, and dialysis centres. In such contexts, these infections are classified as healthcare-associated MRSA (HA-MRSA).
HA-MRSA infections are frequently linked to invasive medical procedures or the utilization of medical devices, such as surgeries, intravenous tubing, or artificial joints. Transmission of HA-MRSA can occur through contact with healthcare workers who have not properly cleaned their hands or by touching contaminated surfaces.
Another variant of MRSA infection occurs in the broader community, affecting individuals who are otherwise healthy. This is known as community-associated MRSA (CA-MRSA).
CA-MRSA infections often initiate as painful skin boils and are typically transmitted through direct skin-to-skin contact. At-risk populations for CA-MRSA include high school wrestlers, gym enthusiasts, childcare workers, and those residing in densely populated conditions.
Causes and Symptoms of MRSA
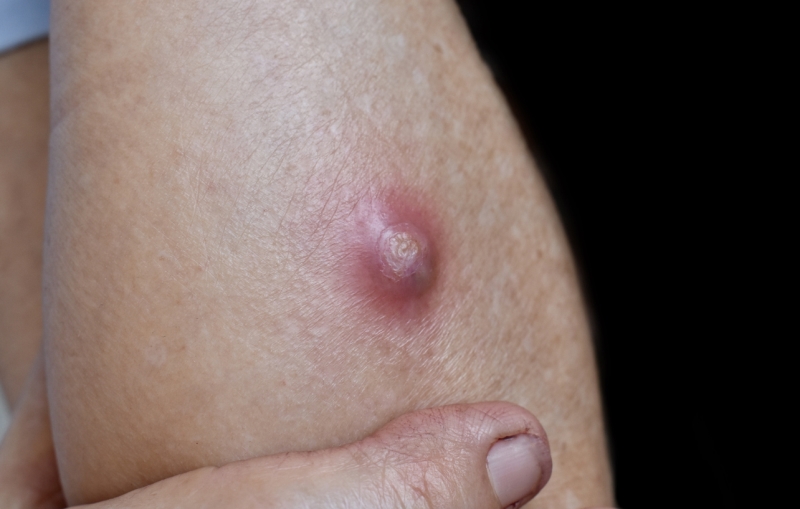
Staph skin infections, including impetigo, typically commence as swollen, painful red bumps resembling pimples or spider bites. The affected area often exhibits the following characteristics:
- The presence of a bump or lump that is swollen and feels firm to the touch.
- Fever, indicating an infection.
- Pain at the site of the bump.
- The discharge of pus from the affected area.
- Increased warmth in the vicinity of the bump and its surrounding area.
On MRSA’s Antibiotic Resistance
The overuse and improper utilization of antibiotics, particularly topical antibiotics, have contributed to the development of antibiotic resistance in staph bacteria. Hence, earning the alias “superbugs.” It stands out as one of the most prevalent strains of antibiotic-resistant staph bacteria, and hospitalizations stemming from MRSA infections are on the rise.
The emergence of staph resistance to topical antibiotics, such as Fucidin and Mupirocin, raises significant concerns for several reasons:
- Staph resistance renders these treatments ineffective, leaving fewer options for managing infections.
- Resistance to one antibiotic often implies resistance to other antibiotics, limiting treatment choices further.
- The growing resistance of staph bacteria to these topical antibiotics jeopardizes the effectiveness of oral and intravenous formulations of these medications, which are crucial for treating severe infections. For instance, oral fusidic acid addresses invasive staph infections affecting bones and joints.
Can Mānuka Oil Kill MRSA?

Research has revealed the exceptional efficacy of East Cape Mānuka Oil in combating various pathogens, including Staphylococcus Aureus, Methicillin-Resistant Staphylococcus Aureus (MRSA), Streptococcus, and pathogenic fungi. This oil exhibits potent antibacterial and antifungal activity, surpassing that of tea tree oil by more than 30 times in laboratory tests. Moreover, mānuka oil has proven effectiveness against numerous microorganisms that commonly affect the skin.
Unlike conventional chemicals that directly kill MRSA, East Cape Mānuka Oil operates through a distinctive mechanism. Research indicates that when MRSA is treated with mānuka oil, it experiences a deficiency in a specific protein essential for synthesizing fatty acids crucial for building and maintaining healthy cell walls. Consequently, the bacteria becomes debilitated, loses its ability to reproduce, and ultimately perishes.
The efficacy of East Cape Mānuka Oil against Staph and MRSA is of significant importance, as it provides an avenue for reducing the overuse of antibiotics.
Mānuka oil encompasses a range of significant components, including alpha-pinene, beta-pinene, myrcene, para-cymene, 1,8-cineole, linalool, methyl cinnamate, alpha-farnesine, isoleptospermone, leptospermone, as well as sesquiterpenes such as cardinal-3,5-diene and delta-amorphene, along with triketones. These constituents are responsible for manuka oil’s antibacterial and anti-inflammatory properties, which are effective against several Gram-Positive bacteria, Gram-Negative bacteria, and Fungi.
| Gram-Positive Bacteria | Gram-Negative Bacteria | Fungi |
| Bacillus subtilis
Micrococcus luteus Sarcina lutea Staphylococcus aureas Staphylococcus aureas (methicillin-resistant) Staphylococcus epidermidis Streptococcus agalactiae Streptococcus faecalis |
Escherichia coli
Klebsielle pneumoniae Proteus vulgaris Pseudomonas aeruginosa Pseudomonas florscens Vibrio fumissii |
Aspergillus niger
Candida albicans Microsporum canis Trichophyton mentagrophytes Trichophyton rubrum |
Source: https://www.mudscuppers.com/East-Cape-Manuka-Oil-s/1861.htm
How To Treat MRSA At Home
Many of the measures employed to treat MRSA also serve as effective preventive strategies. In cases where one has contracted MRSA, it is likely that the bacteria has colonized or multiplied in larger numbers on the skin and may have also spread to various objects within the home.
The primary objective of at-home treatments is to decolonize MRSA, thereby reducing the quantity of bacteria and minimizing the potential for reinfection. Here are steps to undertake for MRSA decolonization:
- Maintain Short Fingernails: Keep fingernails trimmed short to prevent scrapes, scratches, and the accumulation of bacteria beneath the nails.
- Regularly Launder Clothing and Personal Items: Wash clothing items and personal items such as towels and washcloths after each use to eliminate any potential bacterial contamination.
- Frequent Washing of Bed Linens: Wash bed linens at least once a week using hot water, ideally exceeding 160°F (71°C). Dry sheets using the highest heat setting available.
- Bathe with Appropriate Cleansers: Bathe using chlorhexidine (HIBICLENS) soap or add a small amount of liquid bleach, typically around one teaspoon per gallon of bathwater. These methods can help remove MRSA from the skin. Note that this may cause excessive dryness, so this cleanser should not be used on individuals with eczema or already dry skin.
- Clean and Cover Cuts, Scrapes, and Sores: Use a mild antibacterial soap to clean cuts, scrapes, and sores. Ensure these open areas are covered with clean, dry bandages until fully healed.
- Refrain from Sharing Personal Care Items: This includes clothing, towels, razors, brushes, combs, and makeup.
Other Mānuka Oil Benefits
A substance long employed by the Māori people of New Zealand, mānuka oil offers a range of applications beyond its efficacy in treating MRSA. Some of its versatile uses include healing:
- Eczema
- Acne
- Psoriasis
- Fungal infections (athlete’s foot, toenail fungus, ringworm)
- Dry skin
- Chafing and Rashes
- Inflammation
- Asthma
- Cough
- Colds
- Insect bites and stings
- Allergies
- Rashes and sores
- Burns
- Dandruff and scalp issues
- Foot and body odour
- Ear infections
- Anxiety
- Joint pain
- Muscle pain
- Pet skin issues for dogs and cats